Skyland Trail is a trailblazer in the area of measurement-based care and outcomes research, which is an integral part of our evidence-based treatment model. Our robust outcomes and research program employs evaluative instruments considered to be the gold standards in the mental health field to measure the effectiveness of our treatment programs.
Outcome data from 2008 through 2019 confirm that our unique integrated, evidence-based approach helps our clients return to their communities with reduced symptoms and improved skills to pursue more independent and productive lives.
2019 AREA OF FOCUS
In 2019, we explored the impact of family therapy on treatment outcomes.
2019 OUTCOMES RESEARCH REPORT
2019 Client Community
Age at Admission
Gender
Primary Diagnosis at Discharge
Patient Complexity
Skyland Trail has specialized in treating complex patients for many years. Many patients enroll in the residential treatment program after participating in other outpatient or inpatient therapeutic programs without results.
In 2019, Skyland Trail treated a large number of young adult patients ages 18 to 25 with a complex constellation of co-occurring disorders: a mood disorder, borderline personality disorder, and a substance misuse disorder. Patients in this category had outcomes similar to the broader patient population and experienced significant improvement in symptoms, functionality, and hopeful thinking.
60% of clients
had >3 co-occurring diagnoses confirmed at discharge
Co-occurring disorders include: anxiety disorders, substance misuse, borderline personality disorder, others
2019 Key Outcomes
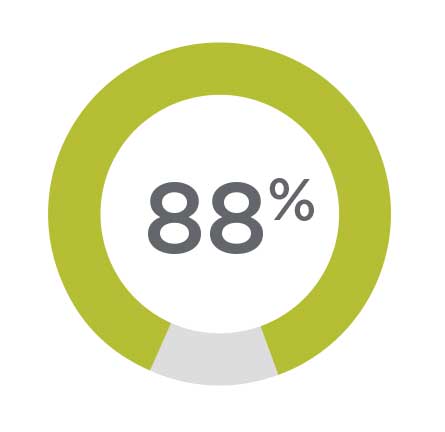
Improved Functioning
88% of all patients
experienced a statistically significant improvement in functionality, symptoms and social relationships 1
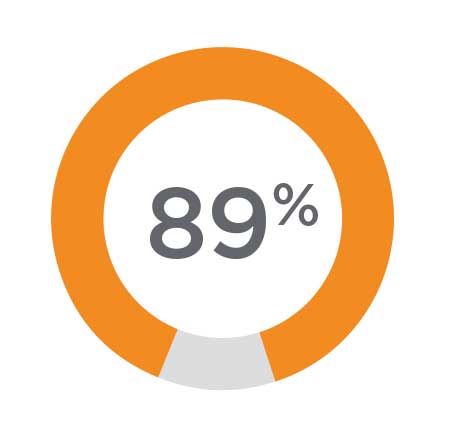
Improved Hope
89% of all patients experienced a statistically significant improvement in hope 2
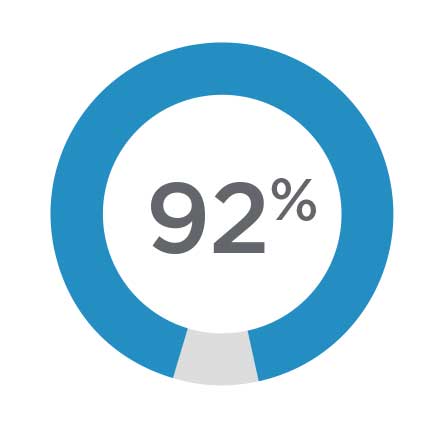
Improved Medication Attitudes
92% of patients leave treatment with a positive attitude about taking psychiatric medication 3
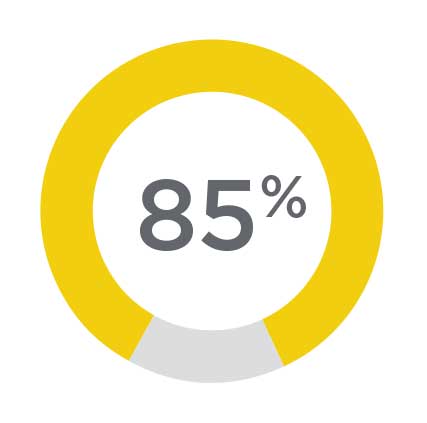
Reduced Psychosis
85% of patients with psychosis experienced statistically significant improvement in their symptoms of psychosis 4

Reduced Depression
89% of patients with very severe and severe symptoms of depression experienced clinically significant reduction 5
Reduced Mania
96% of patients who had clinically meaningful episodes of mania showed no symptoms of clinically meaningful mania at discharge 6
(1) The 32-item Behavior and Symptom Identification Scale (BASIS-32): ©McLean University, Affiliate of Harvard Medical School. (2) Beck Hopelessness Scale: Beck AT, Weissman A, Lester D, Trexler L. (1074). The measurement of pessimism: The Hopelessness Scale. Journal of Consulting and Clinical Psychology, 42(6), 861-865. (3) Medication Attitude Inventory: Hogan TP, Awad AG, & Eastwood R. (1983). A self-report scale predictive of drug compliance in schizophrenics: reliability and discriminative validity. Psychological Medicine, 13, 177-183. (4) Overall JE, Gorham DR. The Brief Psychiatric Rating Scale. Psychological Reports. 1962; 10:799-812. (5) Montgomery, S.A. & Åsberg, M. (1979). A new depression scale designed to be sensitive to change. British Journal of Psychiatry, 134, 382-389. (6) Young RC, Biggs JT, Ziegler VE, Meyer DA: A rating scale for mania: reliability, validity and sensitivity. British Journal of Psychiatry, 133:429-435, 1978. (7) Hamilton M: The assessment of anxiety states by rating. British Journal of Medical Psychology, 32:50-55,1959.
Symptom Reduction
Skyland Trail administers disease-specific outcome measurement tools every two weeks of treatment, based on the confirmed diagnosis at admission. Though the scales differ for each measurement, lower scores always indicate improved symptomatology.
MAJOR DEPRESSION
89% of patients with very severe and severe symptoms of depression experienced clinically significant reduction
t(222)= 10.30, p=0.000
Montgomery, S.A. & Åsberg, M. (1979). A new depression scale designed to be sensitive to change. British Journal of Psychiatry, 134, 382-389.
Montgomery-Asberg Depression Rating Scale 2019
BIPOLAR ILLNESS
96% of patients who had clinically meaningful episodes of mania showed no symptoms of clinically meaningful mania at discharge
t(25)= 4.42, p=0.001
Young, et. Al. (1978). A rating scale for mania: reliability, validity, and sensitivity. British Journal of Psychiatry, 133, 429-435.
Young Mania Rating Scale 2019
ANXIETY DISORDERS
89% of patients with anxiety experience statistically significant improvement in control of anxiety
t(202)= 6.44 p=0.000
Hamilton M: The assessment of anxiety states by rating. British Journal of Medical Psychology 32:50-55,1959.
Hamilton Scale of Anxiety 2019
THOUGHT DISORDERS
85% of patients with psychosis experienced statistically significant improvement in their symptoms of psychosis
t(46)= 11.8, p=0.000
Overall JE, Gorham DR. The Brief Psychiatric Rating Scale. Psychological Reports. 1962; 10:799-812.
Brief Psychotic Rating Scale 2019
All Client Assessments
These assessments are administered to clients with all diagnoses at admission and at discharge.
IMPROVED FUNCTIONING
In 2019, patients consistently showed statistically significant functional improvement as measured by the BASIS-32. Comprised of 5 subscales, the BASIS-32 contains an overall average score ranging from 0 to 4, with lower scores indicating greater levels of functioning in daily life, interpersonal relationships, impulsivity, psychosis, depression, and anxiety.
Clients as a group showed significant impairment at admission, and low-moderate impairment (and in many cases, no impairment) at discharge.
The 32-Item Behavior and Symptom Identification Scale (BASIS-32). © Copyright McLean University, Affiliate of Harvard Medical School.
Significant Impairment
>1.5 Significant and systemic impairment in daily life and/or interpersonal relationships, with extreme impulsivity, psychosis, depression, and/or anxiety present.
Moderate Impairment
.5–1.5 Moderate impairment in daily life and/or interpersonal relationships, with some impulsivity, psychosis, depression, and/or anxiety present.
Full Functioning
<0.5 Indicates full functioning with no significant impairment in daily life and/or interpersonal relationships, with little or no impulsivity, psychosis, depression, and/or anxiety present.
BASIS-32 Overall Change Scores 2019
T(203) = 15.965, p = 0.000
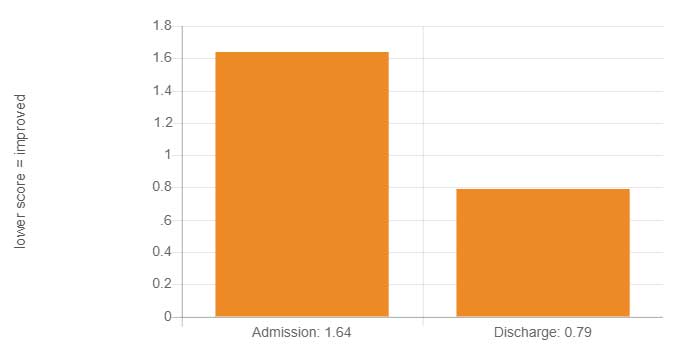
BASIS-32 Subscales Change Scores 2019
Relation to Self/Others
t(203) = 15.783, p = 0.000
BASIS-32 Subscales Change Scores 2019
Depression/Anxiety
t(203) = 15.243, p = 0.000
BASIS-32 Subscales Change Scores 2019
Daily Living Skills
t(203) = 8.050, p = 0.000
BASIS-32 Subscales Change Scores 2019
Impulsivity
t(203) = 8.050, p = 0.000
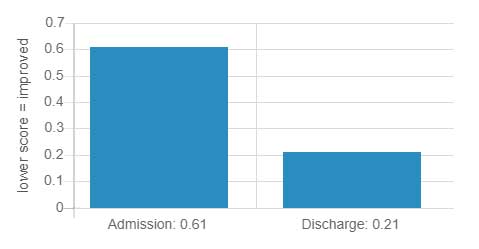
INCREASED HOPEFUL THINKING
In 2019, clients continued to experience a statistically significant decrease in feelings of hopelessness, t(198) = 12.399, p=0.000. This finding indicates that, on average, individuals improved from feeling very hopeless at admission to having hopeful future expectations at discharge. Hope for one’s future is one of the best predictors of continued adherence to a recovery plan and protective against suicide.
Human beings are much more than constellations of symptoms, thoughts and behaviors. Hopefulness, social interconnectivity, and a sense of self efficacy define recovery and what it means to be mentally well.
Beck AT, Weissman A, Lester D, Trexler L. (1974). The measurement of pessimism: The Hopelessness Scale. Journal of Consulting and Clinical Psychology, 42(6), 861-865
Nihilistic Preoccupations
>8 These individuals see very little hope in all domains of their lives.
Some Hopelessness
3–8 Individuals display some hopelessness in their thinking. Individuals closer to 8 can be said to be very hopeless while those scoring closer to 3 can be said to be somewhat hopeless.
Hopeful
<3 Individuals are said to be hopeful.
Beck Hopelessness Scale Scores 2019
t (198) = 12.399, p=0.000
IMPROVED MEDICATION ADHERENCE
Attitude toward taking psychiatric medications is a surrogate measure for medication adherence. Medication adherence is one of the best predictors of sustained recovery.
Scores on the Medication Attitude Inventory (MAI) range from -10 to +10, with higher scores indicating more positive attitudes towards medication use and medication adherence. On average, clients in 2019 experienced very highly statistically significant improvement with an average attitude score of 4.47 at admission to a 7.10 at discharge.
Hogan TP, Awad AG, & Eastwood R. (1983). A self-report scale predictive of drug compliance in schizophrenics: reliability and discriminative validity. Psychological Medicine, 13, 177–183.
>5 Indicates generally positive attitudes towards medication use and are correlated with greater levels of medication adherence in a clinical setting.
Medication Attitude Inventory 2019
t (205) = -9.009, p=0.000
IMPROVED ABILITY TO MAKE DECISIONS
A sample of 204 clients who completed the Making Decisions Scale at admission and discharge demonstrated statistically significant improvement in their ability to use self-esteem, optimism, and personal power in making decisions.
A four-point scale, where scores centered around 1 indicate negative beliefs about the ability to make decisions with psychological components like:
• self-esteem
• optimism
• activism
• personal power (beliefs in the efficacy to make decisions on one’s own)
Rogers et al. (1997). A consumer-constructed scale to measure empowerment among users of mental health services. Psychiatric Services, 48(8), 1042-1047.
Making Decisions Scale 2019
SELF-ESTEEM
t(203) = 8.050, p = 0.000
OPTIMISM
t(203) = -7.948, p = 0.000
ACTIVISM
t(203) = -2.887, p = 0.004
PERSONAL POWER
t(203) = -8.521, p = 0.000
2019 Highlight: Impact of Family Engagement
In 2019 Skyland Trail examined factors that influence adult patients' engagement in treatment and their likelihood to complete treatment with statistically and clinically significant reduction in symptoms and improvement in functioning.
This analysis pointed to the importance of family and support system engagement as a key variable, especially for adult patients with complex diagnoses. Skyland Trail engages families in treatment through several programs.

Family Orientation
On average, about 48% of families attend family orientation. Family orientation is a full-day education and information session presented by several members of the clinical team. In addition to an overview of how clients move through the treatment program, families learn how programs like family therapy, vocational services, and expressive therapies contribute to their loved one's recovery.

Family STEP
The Family STEP program is a weekly education and peer support group for families. Families can participate in person or through zoom online conferencing. Skyland Trail clinical team members as well as experts from the community present on a variety of topics from mindfulness to pharmacology. The number of STEP services delivered increased 35% from 2017 to 2019.

Family Therapy
Family therapy with our family psychologist is offered to adult residential and day treatment clients. Family therapy with our adolescent family therapist is an integrated part of our adolescent residential and day treatment programs.
Last year, participation in family therapy in our adult programs grew from 40% (N=302) in 2018 to 50% in 2019 (N=276).
Adult Clients Who Graduated (Completed Program)
Adult Clients Who Did Not Graduate
Family Therapy Impact on Symptoms
- On average, adult clients in 2019 who participated in family therapy experienced a 7% greater improvement in feelings of hope than clients who did not participate in family therapy.
- Adult patients with depression and thought disorders who graduated (completed treatment) but did NOT attend family therapy did not, on average, reach the same level of symptom reduction as the patients who attended family therapy.
Family Therapy Impact on Program Completion
- Adult patients who do NOT participate in family therapy have 4.2X greater odds of leaving treatment before graduation (treatment completion).
Adult Programs Family Therapy
Family therapy, led by family psychologist Carlyle Bruce, PhD, is available to adult clients in residential treatment and day treatment. Family therapy is available via zoom online conferencing.
Adolescent Family Therapy
The Adolescent Family Program provides an orientation to the Skyland Trail treatment program, education on relevant mental health topics, and structured peer support for parents and guardians of clients currently enrolled in the adolescent treatment program. The program is offered at no cost to parents and guardians. Learn More.

