Do I Have to Take Medications to Manage My Mental Illness?
Evidence-based Medication Management & Education at Skyland Trail
A key tenet of the Skyland Trail treatment philosophy is that mental illnesses are medical problems. And just like with other medical problems, people with a psychiatric disorder often require medications to feel their best and live a healthy life.
A commitment to take medications for a chronic illness – whether diabetes or major depressive disorder – can feel daunting. Various sources on the internet question the necessity or even prudence of using medications to treat illnesses like depression or anxiety, the symptoms of which are sometimes harder to measure than blood sugar or cholesterol levels.
Further, just as with other illnesses, patients will see the best results when medications are prescribed and taken properly. People living with mental illness may face more challenges in identifying the right medication strategy and adhering to it over time. Poor prescribing and adherence leads to bad outcomes, which can give psychiatric medications a bad reputation.
The decision of whether or not to take psychiatric medication is ultimately a decision for the patient to make in partnership with their physician. Decisions informed by the current foundation of research on best practices in prescribing, patient education, and adherence strategies will yield the best long-term outcomes for patients and likely prevent adverse reactions and side effects that make some people skeptical about the utility of psychopharmacology.
Which Mental Illnesses Require Medication?
There are some psychiatric diagnoses for which medications are particularly important, including bipolar mania and schizophrenia. People with these diagnoses who receive treatment that includes medications have better outcomes. These illnesses are typically quite responsive to medications, so symptoms resolve more quickly. And the reduction of symptoms related to these diagnoses is more dependent on medications; no other treatments have proven to be as effective on their own.

Medications are particularly important for people with bipolar mania and schizophrenia
Further, the consequences of both untreated mania and untreated schizophrenia can be profound. Individuals with these two illnesses have the highest rates of completed suicides of all mental illnesses. People experiencing mania can behave impulsively and make poor decisions with long-term detrimental consequences to their health, relationships, and financial situations.
There is general consensus that for every day that someone with these diagnoses goes without medication treatment (often termed duration of untreated psychosis or “DUP”), there are many biological changes in the brain and body that make long-term recovery less possible. Without that biologic intervention (i.e. medication), the prognosis for getting better for someone with bipolar mania or schizophrenia goes down, and, therefore, introducing effective medications as soon as possible for these individuals is critical.
Are Medications Required to Treat Depression?
While some people with depression manage their illnesses without prescribed medications, medications can be an important tool in reducing symptoms and regulating mood, especially when combined with psychotherapy. Studies involving adults with moderate to severe depression indicate that medications improved depression symptoms for many participants. And adhering to medications over time has been shown to help prevent relapse. This is particularly important because relapses with depression are very common without ongoing preventive treatment and actually become more likely with each recurrence.
Which Mental Health Diagnoses Do Not Respond to Medication?
For most mental illnesses, there is a role for biologically manipulating what is going on in the brain using psychiatric medications. However, a counter-example of that is the treatment of personality disorders like borderline personality disorder. Currently, no psychiatric medications have been identified that effectively treat the core of why someone has developed a personality disorder.

Currently, no psychiatric medications have been identified that effectively treat the core of why someone has developed a personality disorder like borderline personality disorder.
A physician may prescribe an antidepressant for someone with borderline personality disorder because they have developed comorbid depression as a result, in part, of having untreated borderline personality disorder over time. But there is no medication that will treat the fundamental issues at the root of borderline personality disorder. This illustrates the importance of combined treatment with evidence-based psychotherapy such as dialectical behavior therapy (DBT).
Are Psychiatric Medications Safe for Teens?
Psychiatrists and families often are more reticent to prescribe psychiatric medications for adolescents. One challenge is that there are very few medications that are FDA approved to treat adolescents. In most cases, this is not because there are known risks for teens taking these medications. Most psychiatric medications have not undergone the clinical tests required to determine efficacy and safety specifically for teen patients because medical trials for children and teens are very difficult to get approved and implemented. In order to be FDA approved, the clinical trials must be completed.
Though physicians may prescribe psychiatric medications for adolescents without FDA approval, lack of FDA approval may contribute to a sense of caution for prescribers and families. However, medications are still an important part of treatment for many teens, particularly adolescents experiencing psychosis or mood or anxiety symptoms that are preventing them from participating fully in school or peer and family relationships. Teens who experience thoughts of suicide or self-harm as part of a mood or anxiety disorder may also benefit from psychiatric medications in important ways.
How Do I determine My Diagnosis and What Treatment I Need?
A thorough assessment from a mental health professional is critical to identifying an effective treatment. Patients admitted to Skyland Trail receive a very thorough assessment to make sure their treatment team has good working diagnoses. Results of the assessment help us tailor an individualized treatment plan that stipulates the relative importance of psychiatric medications, psychotherapy and interpersonal therapy, and other elements of our treatment program based on what the individual is likely to respond to best.
How Many Medications Are Too Many?
While there is no singular correct answer to this question, there is a consensus on the best process to answer it for each patient. In the research literature, the process is called conducting an “adequate trial.” An adequate trial has four components: dosing, timing, duration, and adherence.

An adequate trial means that the physician has selected an appropriate medication, dosed it correctly, and waited enough time or made appropriate adjustments within a reasonable window of time to produce the best results. An adequate trial also requires that the patient has taken the medication as prescribed.
An adequate trial means that the physician has selected an appropriate medication, dosed it correctly, and waited enough time or made appropriate adjustments within a reasonable window of time to produce the best results. Research studies are crucial to understanding the specifics of any adequate trial and a skilled prescriber will know and understand the evidence from research to guide their recommendations. An adequate trial also requires that the patient has taken the medication as prescribed. If you don’t meet all four of those variables, you cannot determine that a medication has or has not worked. You need to meet all four variables to maximize the potential benefit of any medication.
Often patients start a medication, do not use the adequate trial approach, and do not experience expected results. When they talk to their prescriber, some prescribers will continue the first medication as part of an inadequate trial and add additional medications. This approach can complicate prescribing. Some medications when taken together have interactions that alter effectiveness. In addition, most medications have side effects, and, when you are taking many medications at once, the compounding side effects may feel really terrible. Patients may find themselves in a situation where they are contending with all the side effects and problems of prescribed medications without experiencing maximum benefit from any one of them. That concept is called “polypharmacy,” and it contributes to a perception that psychiatric medications are overprescribed.
How Do I Find the Right Medication for Me?
Typically at Skyland Trail, we stop more medications for our patients than we start. Many patients enter Skyland Trail with several prescribed medications and report that none of them is really working. We often are able to reduce the overall number of medications a client is prescribed by taking an evidence-based approach with the medications we have confidence will work when given an adequate trial.
After a patient is assessed, Skyland Trail psychiatrists pick one medication that is indicated to treat the identified diagnosis and then take a very evidence-based approach in terms of the dosing, timing, duration, and adherence.
The dosing component of an adequate trial can be very nuanced. Working with a physician with specialized experience in treating mental illnesses often yields the best results. Skyland Trail psychiatrists stay up-to-date on research studies and participate in clinical training to ensure they have the best information on appropriate dosing. Patients with a history of medication “failures” often have been prescribed appropriate medications but without proper dosing or patient adherence.
For example, to treat a person diagnosed with generalized anxiety disorder (GAD), picking an appropriate medication out of the SSRI class is relatively straightforward based on targeted symptoms, side effect profiles, and other variables such as insurance coverage or price. However, research indicates that, in order for an SSRI to work for someone with a diagnosis of GAD, you have to start at a lower dose than you would if you were prescribing the same medication for someone with a diagnosis of depression. Further, you have to transition slowly over time to a higher therapeutic dose than you would prescribe for a person with depression. If the medication is not prescribed and taken appropriately, you can be on the right medication, but it’s not going to help with your generalized anxiety disorder.
Typically, if an adequate trial does not produce good results, Skyland Trail psychiatrists stop the medicine and move on to another medicine using the same approach. If a medication succeeds in reducing one set of symptoms, and the patient continues to experience other symptoms related to the primary or a co-occurring diagnosis, additional medications may be added.
If no medications adequately alleviate symptoms, other nonpharmacological treatments like transcranial magnetic stimulation (TMS) may be recommended. Additionally, evidence-based psychotherapy along with healthy lifestyle choices are essential components of every treatment plan.
How Does Residential Treatment Help with Medication Management?
Residential treatment may be especially helpful for patients struggling to find the right medication strategy. Patients are observed by an entire multidisciplinary team of clinical professionals 24/7 who can provide feedback to the prescribing psychiatrist. For example, group counselors may comment that a patient had difficulty sitting still in group therapy and needed to pace. Art or music therapists may provide feedback that a patient was lethargic, had trouble staying awake in a group, or seemed to have trouble concentrating. Even when a patient is less able to articulate their experience with a medication, the psychiatrist can combine the patient’s reported experience with feedback from the clinical team to pivot more nimbly and make meaningful adjustments to medications in real-time.
Residential treatment may be especially helpful for patients struggling to find the right medication strategy.
Residential patients also are administered medications by the residential nursing team, which helps ensure that the patient adherence variable of the adequate trial process is met. While patients always have the right to refuse medications, nurses help ensure the correct dose of the medication is taken on the prescribed schedule and document any unexpected deviations. This helps ensure the patient and prescriber have all the data needed to determine if a medication is working.
Similarly, if residential patients are struggling with their symptoms and need expedited medication adjustments, those changes can happen very quickly, even overnight. Research shows that assertive treatment produces better results and prognoses for recovery than delayed medication prescribing.
What Role Do Prescribers Play in Improving Medication Adherence?
Data suggest that many patients with diagnosed mental illnesses are not adherent to their prescribed medications. Many theories have been proposed to explain this. Some patients, especially younger people, are reluctant to accept that they have a chronic medical problem. Embracing the idea that you may have to take medications two to three times a day for the rest of your life is not always an appealing idea, even when you know they help you stay healthy. Some medications also have side effects like weight gain, sexual dysfunction, or hair loss, that are, understandably, deterrents to daily use.
A recent study suggests another possible contributing factor to poor medication adherence. The study looked at all the factors known to contribute to medication non-adherence in patients with bipolar disorders. People diagnosed with bipolar disorders have one of the highest rates of non-adherence. In the study, over half of patients missed at least one dose of their prescribed medications in the 30 days prior to the assessment. When interviewed, the majority of patients reported that a primary contributing factor to their non-adherence was that they felt that the prescriber did not know them well enough or did not have their best interests in mind to make a prudent medication recommendation.

Prescribers who also engage in psychotherapy with their patients may contribute to an improvement in medication adherence and therefore an overall improvement in symptoms and functionality.
Improved attitudes about taking medications cultivated through psychotherapy is another example of how building rapport and trust with a patient is crucial to helping them get better. Prescribers who also engage in psychotherapy with their patients may contribute to an improvement in medication adherence and therefore an overall improvement in symptoms and functionality. You can be a brilliant pharmacologist, but, if you don’t cultivate a therapeutic alliance with your patients, your patients may still experience poor outcomes because they may be less likely to take the medications you prescribe.
While Skyland Trail patients meet individually with a specialized primary therapist, they also meet weekly with their psychiatrist and engage in psychotherapy and discussions about their medications. The psychiatrist and primary therapist also communicate closely to ensure everyone has a full picture of the patient’s goals for treatment and ongoing challenges.
How Can Prescribers Help Patients Think About Medications More Positively?
Psychoeducation also is a key component of the treatment program at Skyland Trail. Psychoeducation includes helping patients understand their diagnoses, what may be happening biologically in their brains and bodies that is related to their symptoms, and how their medications work to counteract or balance those biological changes. Patients who have a more complete understanding of what medications they are taking and why tend to have a better attitude about taking medications.
Physicians educate patients about potential side effects in advance so that they are not surprised or concerned if those side effects occur. Patients learn how long those side effects typically last, how to mitigate them if possible with lifestyle changes or other medicines, and when to seek help for serious concerns.
Our nursing team also works with patients individually to help them learn to fill and maintain a medication box before patients graduate from residential services and start day treatment. As part of the education, patients are encouraged to learn the names of their medications, recognize them by sight, understand their purpose, and know how to follow the dosing instructions on the pill bottle or package.
Skyland Trail patients complete the Medication Attitude Inventory assessment, a standardized and normed evaluation, at admission and at discharge. The majority of patients have both a clinically and statistically very-highly significant improvement in their attitude toward taking medications after completing treatment at Skyland Trail. A positive attitude about taking medications can be a good predictor of long-term medication adherence.
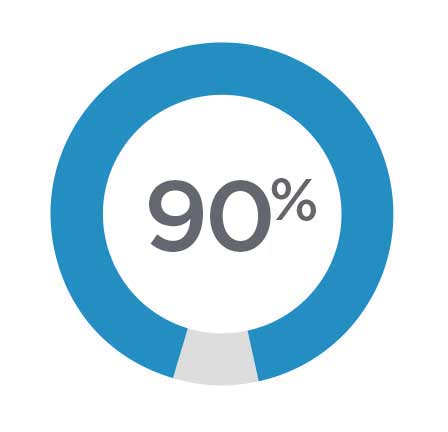
In 2020, 90% of adult Skyland Trail patients left treatment with a positive attitude about taking psychiatric medication
What Medical Advancements Are Improving Medication Adherence?
Improving medication adherence among people with anosognosia continues to be a challenge for the medical community, patients, and families. Anosognosia is the clinical term used when someone is unaware of their own mental health condition or does not have the insight to perceive their condition accurately. Patients with schizophrenia or who experience psychosis as a symptom of other disorders often have anosognosia. This creates a tremendous challenge for recovery.
People with schizophrenia or psychosis require pharmacologic treatment to get better. However, the chances of someone with anosognosia being able to take a pill twice a day every day for the rest of their lives are almost nonexistent. To improve adherence for people with anosognosia and others, researchers have been working to develop long-acting injectable medications. Administered in a doctor’s office or clinic, one dose can last up to six months. These long-acting injectables have been a game-changer for many people who are challenged by anosognosia.
Skyland Trail helps many patients stay current with their long-acting injectable medications even after they leave the treatment program through our Glenn Family Wellness Clinic.
What Questions Should I Ask My Healthcare Provider About Psychiatric Medications?
Medications are important tools in managing most psychiatric illnesses. They are, in fact, critical for some diagnoses like bipolar mania or schizophrenia. And while there are best practices in the prescribing of medications, arriving at the best medication strategy for you can be a nuanced trial-and-error process. It is therefore important to select and build a relationship with a mental health prescriber you trust.
Consider asking a potential prescriber these questions:
- What is my working diagnosis? And how did you arrive at that conclusion?
- Do you recommend any additional psychiatric assessment or psychological evaluation?
- What is your approach to medication selection and dosing?
- How would you help me manage any side effects?
- Will we engage in psychotherapy?
- How can I best provide feedback to you about my experience with medication changes? Are there opportunities for people in the family to record feedback as well?
- Are you willing to educate me about how medications work in the body and why they may help me?
- Will you provide recommendations for lifestyle changes and other therapies that may contribute to my recovery and overall health?
Having a trusting relationship with a prescriber and a positive attitude about taking medications when appropriate can be a protective factor against relapse and chronic symptoms of many mental illnesses.
When Should I Consider Residential Treatment?
Residential treatment may be an appropriate next step for adults or teens who are not making progress in outpatient therapy or who are leaving an inpatient acute facility. Residential treatment can help patients clarify their diagnoses and develop an effective medication strategy. Talk to your healthcare provider about how residential treatment may be appropriate for your current needs or contact the Skyland Trail admissions team.
